I Took Lady Gaga’s Advice and Attended Mental Health First Aid Training and Here’s What I Thought

This guest blog originally appeared on the UMass Medical School Transitions to Adulthood Center for Research’s parent blog and is posted here with permission.
On Friday, August 16th 2019, I attended the Mental Health First Aid Training offered for free by American Foundation for Suicide Prevention (AFSP) through Lowell Memorial General Hospital. Stephanie Sunderland-Ramsey our trainer is a Prevention Program Coordinator at Wayside Youth & Family Support Network an organization that also offers many trainings here in Massachusetts. Although I’ve done volunteer work for many years around mental health and have family members with lived experience, I figured there might be something new to learn. And since Lady Gaga is a big fan and encouraging us to #BeTheDifference, I decided to go for it. In the course description, it says, “Just as CPR helps you assist an individual having a heart attack, Mental Health First Aid helps you assist someone experiencing a mental health or substance use-related crisis. In the Mental Health First Aid course, you learn risk factors and warning signs for mental health and addiction concerns, strategies for how to help someone in both crisis and non-crisis situations, and where to turn for help.”
Here are some of my thoughts from the 6+ hours I sat in that room at Lowell Memorial Hospital.
First, in the USA, there are 2 versions of this training. One is geared towards providing mental health first aid to adults and the second is geared towards providing aid to young people. I took the one for assisting young people as my focus has always been intervention as early as possible. The handbook is aptly named, “Mental Health First Aid USA – For Adults Assisting Young People.” (Pipe cleaners to keep my hands busy during the day kept my mind engaged.)
The whole idea of mental health “first aid” training is similar to when I learned First Aid as a Girl Scout. It does not expect you to “solve” a problem, but just to provide the first line of “aid” until more help can come along. That means that if someone is suicidal, I wasn’t being trained to provide therapy to help them solve their problems, but rather to know how to handle the current situation and get the right help in place. And I feel like I got that!
My training had about 25 people in it and we came from all backgrounds. There was a children’s librarian who shared that children confess to her all sorts of things they don’t want to tell their parents. There were grandparents who wanted to be better educated on how to help their grandchildren living with mental health conditions. There were people that worked in the mental health field, and there were young adults who want to be advocates and better able to support their friends when they are in crisis.
MHFA began in Australia, and the mascot of the program is a koala bear named ALGEE. That name can help you remember the Action Plan to use when MHFA is needed.
Like “regular” first aid, there are specific steps you can take when someone is having a mental health crisis. Remember A-B-C when it comes to CPR (more recently changed to C-A-B BTW.) Now there’s ALGEE.
Mental Health First Aid Steps
Assess for risk of suicide or harm (including asking the hard questions below).
When someone is going through a mental health crisis, look for signs of suicidal thoughts and behaviors, non-suicidal self-injury, or other harm. Some warning signs we discussed are:
- Threatening to hurt or kill oneself
- Talking or writing about death, dying, or suicide
- Feeling hopeless
- Acting recklessly or engaging in risky activities
- Increased use of alcohol or drugs
- Withdrawing from family, friends, or society
- Appearing agitated or angry
- Having a dramatic change in mood
Next, ASK them if they are suicidal. Mostly everyone in my training agreed that this first item is the toughest. We learned that it is IMPORTANT and CRITICAL to ask, “Are you thinking of suicide?” or “Do you want to kill yourself?” or “Are you going to hurt yourself?” Or something along those lines. I think so many people are afraid to ask those questions. Maybe we are afraid that we are going to give someone an idea that they didn’t have. Or maybe we are too scared to hear the answer. In either case, it is hard to do this. So we practiced. We paired up with someone else and asked those questions. Repeatedly. Practicing saying those words turned down the power of them a bit and by the end it was easier to spit them out. I found this really helpful. I actually went home that night and asked my young adult child those questions (and I had been avoiding them.)
Listen nonjudgementally.
Are you a good listener? It’s a skill that takes practice and it includes body language, eye contact, and acceptance. We learned more details and practiced listening in a way that would help a person feel accepted, respected and understood.
Give reassurance and information.
This might mean explaining that the panic attack will pass and encouraging your person to follow you in breathing or grounding exercises to lessen the panic attack. Or it might mean letting them know you will stay with them and won’t leave them until more help arrives. This piece is focused on helping a person focus on the here and now. But also, it’s so important to reassure someone that mental illnesses and addictions are real, treatable illnesses from which people can and do recover.
Encourage appropriate professional help.
There are many professionals who can offer help when someone is in crisis or may be experiencing the signs and symptoms of a mental illness or addiction. When I practiced this skill, it was asking if my person had a therapist and if we could call together to set up an appointment.
Encourage self-help and other support strategies.
Individuals with mental illness can contribute to their own recovery and wellness through:
- Exercise
- Relaxation and meditation
- Participating in peer support groups
- Self-help books based on cognitive behavioral therapy
- Engaging with family, friends, faith, and other social networks
Theoretically, we all know this, but it’s hard to put into practice. In this training I got support around helping people brainstorm ideas here. Mental Health First Aid helped me identify potential sources of support and practice offering these supports to the person you are helping.
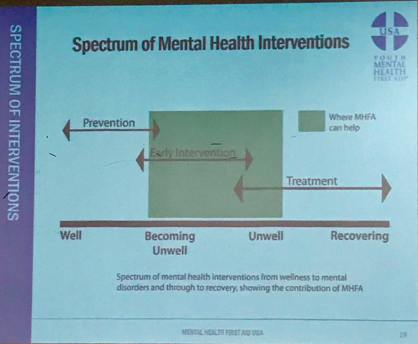 Where does MHFA fit in the spectrum of mental health interventions? This slide offered a good explanation. Prevention is always the best possible situation. But when someone starts becoming mentally unwell, the early intervention skills I learned in this class may help accelerate treatment and recovery. That’s my goal and that’s the goal of MHFA. Mental Health First Aid teaches about recovery and resiliency – the belief that individuals experiencing these challenges can and do get better, and use their strengths to stay well. In many places it’s a free program, and I recommend that we all take the class.
Where does MHFA fit in the spectrum of mental health interventions? This slide offered a good explanation. Prevention is always the best possible situation. But when someone starts becoming mentally unwell, the early intervention skills I learned in this class may help accelerate treatment and recovery. That’s my goal and that’s the goal of MHFA. Mental Health First Aid teaches about recovery and resiliency – the belief that individuals experiencing these challenges can and do get better, and use their strengths to stay well. In many places it’s a free program, and I recommend that we all take the class.
Finally, I just want to show my favorite image of my day. Our trainer, Stephanie Sunderland-Ramsey made a comment that really struck me. I am paraphrasing here, but we were talking about what mental wellness actually IS, and she said something along the lines of, “I know it sounds sappy, like the signs that you often see, but the truth is, that what we all want is just to be able to live, laugh, love and play.” It’s what we aspire to, right? And that is the goal of Mental Health First Aid, to give everyone that chance.
About Transitions ACR:
Transitions to Adulthood Center for Research located in UMass Medical School’s Psychiatry Department is a group of researchers, clinicians and young adults who want to improve the lives of Youth and Young Adults living with mental health conditions. They do research to understand and establish better ways to support this population in their education and job goals, and translate the results into knowledge which they then share with a mixed audience of researchers, service providers, policy-makers, young adults and family members. Transitions ACR’s mission is to promote the full participation in socially valued roles of transition-age youth and young adults (ages 14-30) with serious mental health conditions using tools of research and knowledge translation in partnership with this at-risk population.


